
Issue 13 Duplex Ultrasound Protocol Post EVAR

Duplex Ultrasound Protocol Post EVAR
Duplex is a first-line, non-invasive modality for post-EVAR surveillance, particularly for:
Non-invasive surveillance to detect endoleaks, assess graft integrity, monitor aneurysm sac behavior, and guide management.
Endoleak detection
Graft patency
Aneurysm sac behavior (expansion vs regression)
1. Protocol Overview
Patient Position
Supine, NPO, with Gas-X, 2 tabs the night before and 2 tab the morning of exam
Right and left lateral decubitus may improve iliac imaging
Slight reverse Trendelenburg can improve sac visualization
Equipment
Curvilinear array transducer (1–5 MHz)
Color Doppler and spectral Doppler modes
2. Protocol and Views
✅ A. Aneurysm Sac
Scan in gray scale (longitudinal & transverse)
Measure maximum anterior-posterior (AP) and transverse sac diameter
Compare with baseline (post-op or pre-op imaging)
>5 mm sac enlargement = suspect endoleak, graft issue or endotension or graft failure
Echolucient zones suggest leak or fluid
Mural thrombus
Wall irregularity or pulseatility
✅ B. Endograft Integrity and Surveillance
Visualize entire main body & both iliac limbs
Use Color Doppler to assess patency
Check for: Migration (compare graft end position to landmarks)
Kinking or stenosis
Limb occlusion (absent or reduced flow)
Disconnection (type III concern)
Check graft position: any signs of migration, kinking, or fracture?
Are all limbs visible? Any occlusion?
✅ C. Color and Spectral Doppler Assessment
Color Doppler:
Look for pulsatile flow within the sac (sign of endoleak)
Use low flow settings for slow leaks (Type II)
Spectral Doppler:
Characterize flow as arterial vs. venous
Identify "to-and-fro" pattern → classic for Type II
Sample proximal & distal ends for high-velocity jets → Type I
May detect low-flow endoleaks missed by CT
3. Surveillance Schedule (Typical)
Post-EVAR Imaging
1 month: CTA ± Duplex
6 months: Duplex
12 months: CTA ± Duplex
Annually if stable: Duplex
Some centers alternate CTA and Duplex for long-term surveillance, especially in favorable anatomy or renal insufficiency.

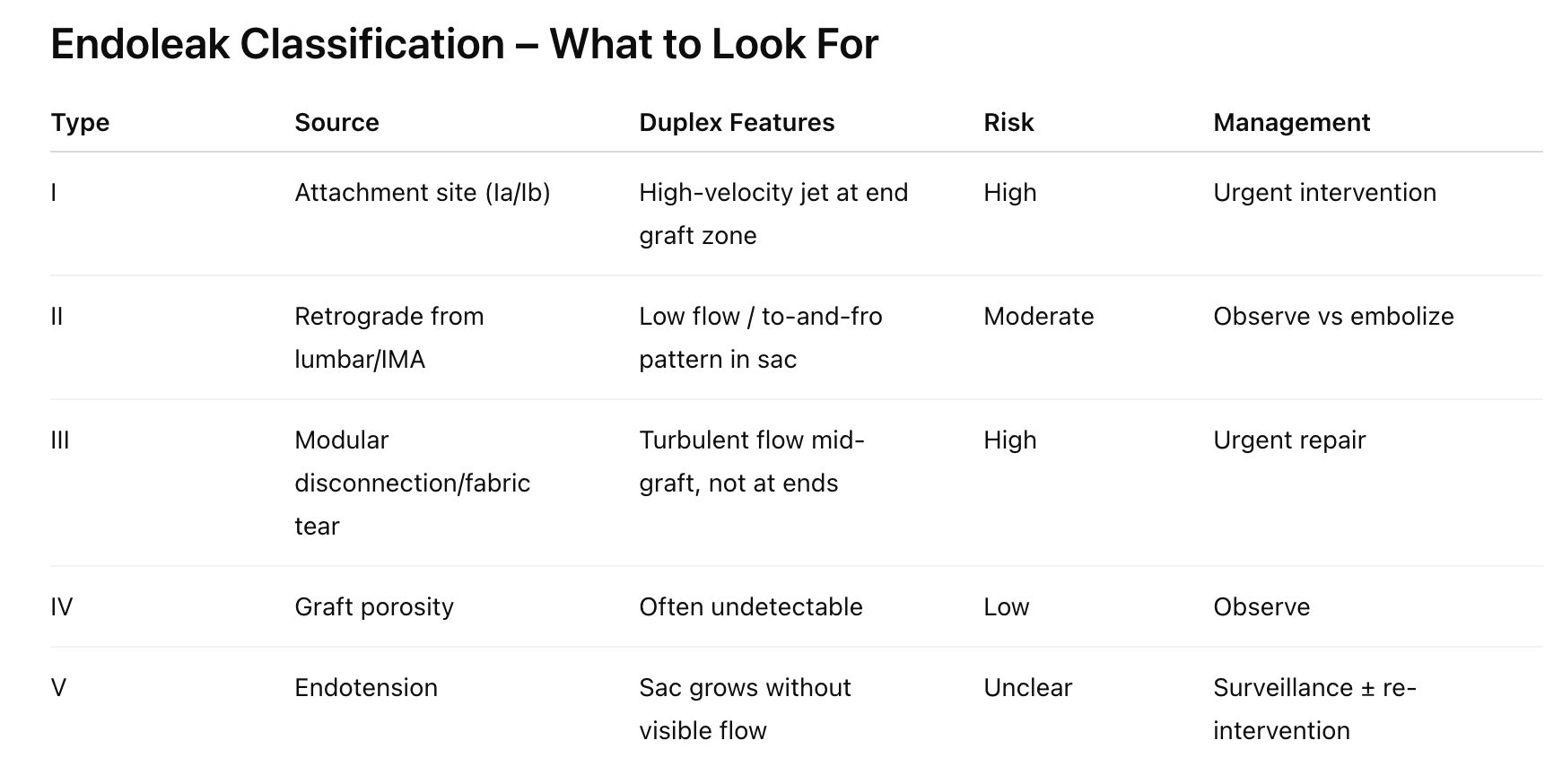
Endoleaks: Types, Appearance, and Management
There are 5 types of endoleaks. Duplex can detect most types, though CTA/CEUS is better in some cases.
Type I – Inadequate Seal (attachment site)
Source: Proximal (Ia) or Distal (Ib) end of graft
Duplex finding: High-velocity flow at graft attachment site entering sac
Risk: High rupture risk
Management: Urgent repair – ballooning, cuff extension, or open conversion
Type II – Retrograde Flow into Sac
Source: Lumbar, IMA, or accessory arteries
Duplex finding: To-and-fro or low-velocity flow into sac; may be delayed
Common? Most common (up to 30–40%)
Management:
Observe unless:
Sac growth >5 mm
Persistent >6–12 months
Then consider embolization (transarterial or translumbar)
Type III – Graft Defect (junction or fabric tear)
Source: Modular disconnection or fabric failure
Duplex finding: High-velocity turbulent flow into sac, not from attachment zones
Risk: High rupture risk
Management: Urgent repair – bridging stents, relining, or open conversion
Type IV – Graft Porosity (rare)
Source: Graft material porosity (seen in older devices)
Duplex finding: Usually not seen – needs CTA
Management: Often resolves spontaneously
Type V – Endotension (no visible leak)
Definition: Continued sac expansion without visible leak
Diagnosis: Diagnosis of exclusion
Duplex finding: No color flow, but sac continues to grow
Management: Controversial: options include open conversion, relining, or continued surveillance
Summary: What to Look for on Duplex Post-EVAR
Flow within aneurysm sac → Suspect endoleak
Enlarging sac >5 mm → Evaluate for Type I, II or III endoleak
High velocity at proximal/distal ends → Suggests Type I
To-and-fro low flow → Classic for Type II
Disrupted graft with turbulent flow → Suggests Type III
Sac growth but no flow → Consider endotension (Type V)
Alert Criteria
Sac growth >5 mm
New or persistent sac flow
Suspicion of Type I/III endoleak
Limb occlusion
Optimization
Goal: Maximize sensitivity for detecting low-velocity, slow-volume flow in or around the aneurysm sac.
1. Grayscale Optimization
Frequency: Use lower frequencies (1–5 MHz) for deep penetration
Depth: Focus just beyond the aneurysm sac
Focal Zone: Set at or just below the sac
Gain: Increase until background noise appears, then reduce
TGC: Brighten posterior sac if needed
Dynamic Range: Wide range to distinguish structures and thrombus
2. Color Doppler Optimization
Key Settings to Adjust:
Color Gain: High (just below noise threshold)
PRF: Very Low (5–15 cm/s)
Wall Filter: Lowest possible
Box Size: Small & focused over sac
Color Map: Use contrast-enhancing maps (red-blue or variance)
Persistence: Medium–high
Steering: Apply to optimize angle relative to graft flow
Tip: Start with a low PRF (~7–10 cm/s), then increase if too much background noise appears.
3. Spectral Doppler Optimization
Sample Gate Size: Small (1–2 mm)
Gain: Increase until background noise, then back off
Sweep Speed: Medium to slow
Angle Correction: Apply only when measuring known flow direction
Look for:
High-velocity jets (Type I/III)
To-and-fro pattern (Type II)
4. Techniques to Enhance Leak Detection
Valsalva Maneuver
Graded abdominal compression
Left lateral decubitus
Reverse Trendelenburg
Re-scan sac after contrast or Doppler delay
CEUS if inconclusive
✅ Quick Troubleshooting Tips
Can’t see sac clearly → Adjust depth, gain, focal zone
No flow detected → Lower PRF, raise color gain
Too much flash/noise → Increase wall filter or decrease gain
Suspected leak but unclear → Try CEUS or delayed scanning
Summary Checklist: Color Doppler Optimization for Endoleak
Color Gain → Max before noise
PRF → As low as ~5–10 cm/s
Wall Filter → Set to minimum
Focus → Centered at sac depth
Box Size → Minimized to target area
Map & Persistence → Chosen for contrast and smoothing
Spectral Sample → Small gate, slow sweep
Dynamic Maneuvers → Valsalva, repositioning
Need help implementing this protocol or training your team?Click here to schedule a customized EVAR ultrasound training or join our community to learn how we can help you and your team.
