# 50 Ultrasound Unlocked

How to Perform and Interpret ABI, Segmental Pressures, and PVR: A Modern Clinical Guide
Noninvasive vascular testing remains the cornerstone of diagnosing peripheral artery disease (PAD). While the fundamentals of testing have not changed, the interpretation and clinical integration have evolved significantly.
The 2024 guideline from the American College of Cardiology and American Heart Association emphasizes a critical shift:
PAD diagnosis should rely on combined physiologic testing, not a single measurement.
This article walks through how to perform and interpret:
ABI
Segmental pressures
Pulse volume recordings (PVR)
The Ankle-Brachial Index (ABI)
How to Perform ABI
The patient should be:
Supine
Rested for at least 10 minutes
Steps:
Measure brachial pressures in both arms
Measure ankle pressures using Doppler:
Posterior tibial (PT)
Dorsalis pedis (DP)
Use the highest ankle pressure
Divide by the highest brachial pressure
Interpretation
1.00–1.40 → Normal
0.91–0.99 → Borderline
≤0.90 → Peripheral artery disease
<0.50 → Severe disease
>1.40 → Non-compressible vessels
Limitations of ABI
Modern practice emphasizes that ABI can:
Be falsely elevated (calcification)
Be normal despite disease
This is why:
ABI must always be interpreted alongside waveform data
Segmental Pressures
How to Perform
Cuffs are placed at:
High and low Thigh
Calf
Ankle
Trans-metatarsal
Each level is measured using Doppler while:
Inflating above occlusion
Slowly deflating
Interpretation
Segmental pressures help identify where disease is located.
Key Rules:
≤20–30 mmHg change = normal
30 mmHg drop = significant disease
20 mmHg difference between legs = abnormal
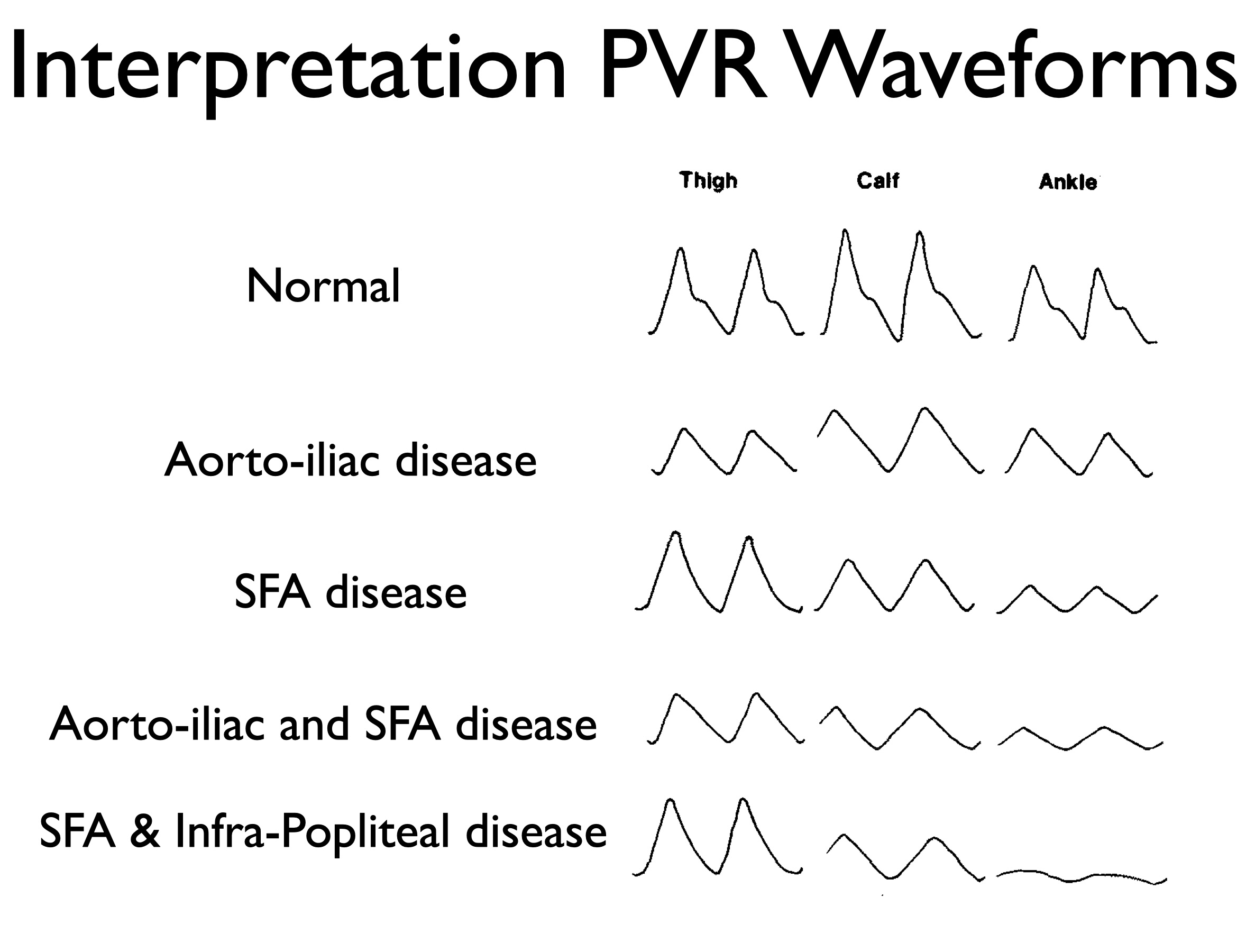
Localization Examples
Decreased thigh pressure → Aortoiliac disease
Drop from thigh to calf → Femoral disease
Drop from calf to ankle → Tibial disease
Pulse Volume Recordings (PVR)
How to Perform
Use same cuffs as segmental pressures
Inflate to ~65 mmHg
Record 3–4 cardiac cycles
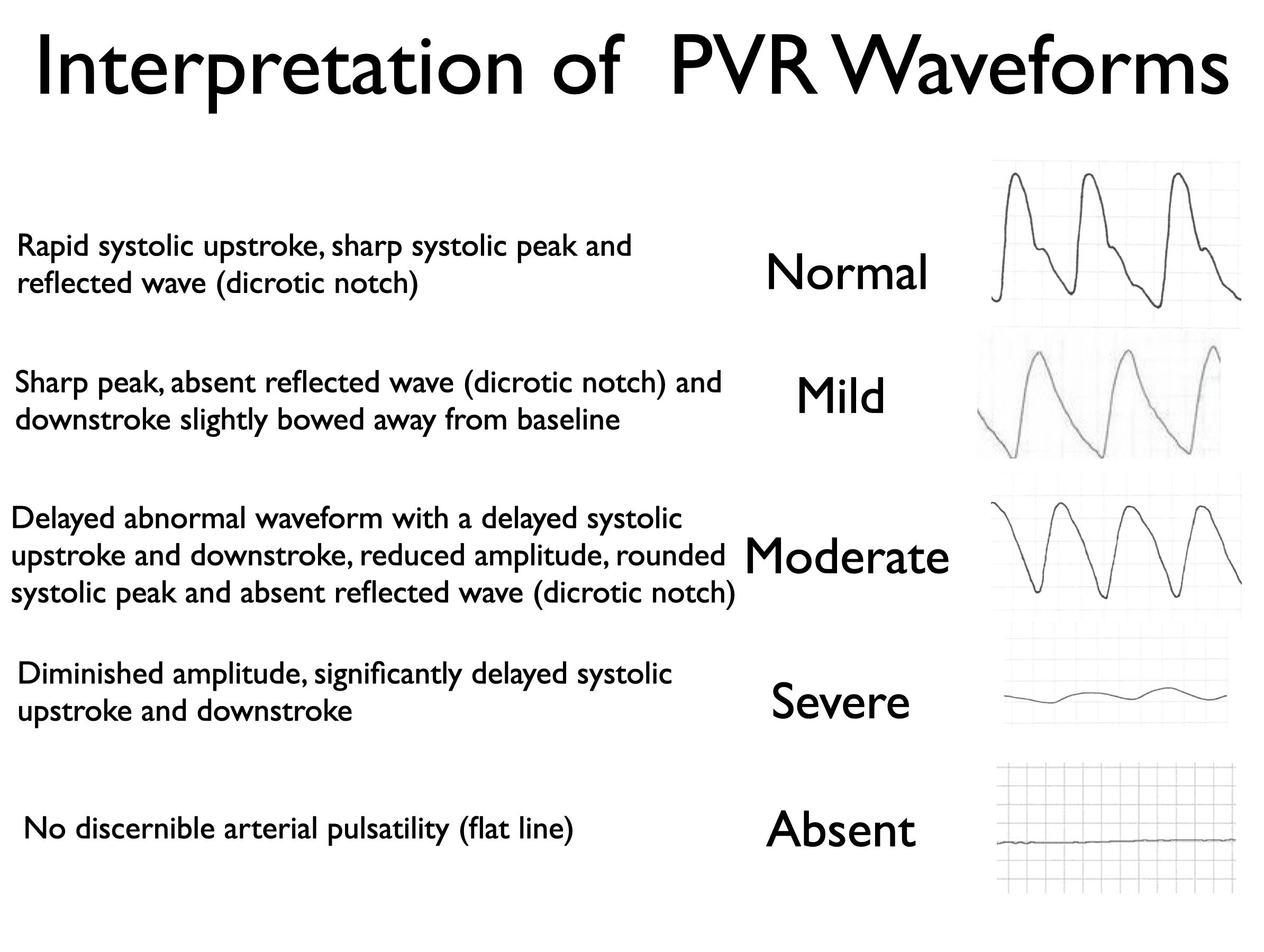
Normal Waveform
A healthy waveform shows:
Rapid upstroke
Narrow peak
Dicrotic notch
Abnormal Waveform
As disease worsens:
Upstroke slows
Peak flattens
Dicrotic notch disappears
Amplitude decreases
Why PVR Matters More Today
PVR is increasingly important because it:
Reflects true blood flow
Is not affected by calcification
Helps confirm or refute ABI findings
In modern vascular labs:
Waveforms often carry more diagnostic weight than pressures alone
Putting It All Together
Modern Diagnostic Approach
Instead of relying on one test, clinicians now integrate:
ABI → identifies disease
Segmental pressures → localize disease
PVR → confirms physiologic impact
Clinical Example
A patient presents with claudication:
ABI: 1.10 (normal)
PVR: dampened waveforms
Segmentals: mild gradient
Interpretation:
Disease is present despite normal ABI
Additional testing is required
My Key Takeaways
ABI remains essential—but not sufficient alone
Segmental pressures help localize disease
PVR provides the most reliable physiologic data
My Final Thought
The future of vascular diagnostics is not about replacing traditional tests - it’s about using them together more intelligently.
Accurate diagnosis now depends on integration, not isolation
