# 51 Ultrasound Unlocked

Catching the Hidden Claudicant – Using Duplex Ultrasound to Unmask PAES
Popliteal artery entrapment syndrome (PAES) is one of those diagnoses that hides in plain sight. The patient is young, often athletic, with exertional calf pain that sounds vascular, but resting ABIs and routine imaging look “normal.” The risk is that these patients get labeled with chronic exertional compartment syndrome or a vague overuse injury, while repetitive arterial compression quietly damages the popliteal artery.
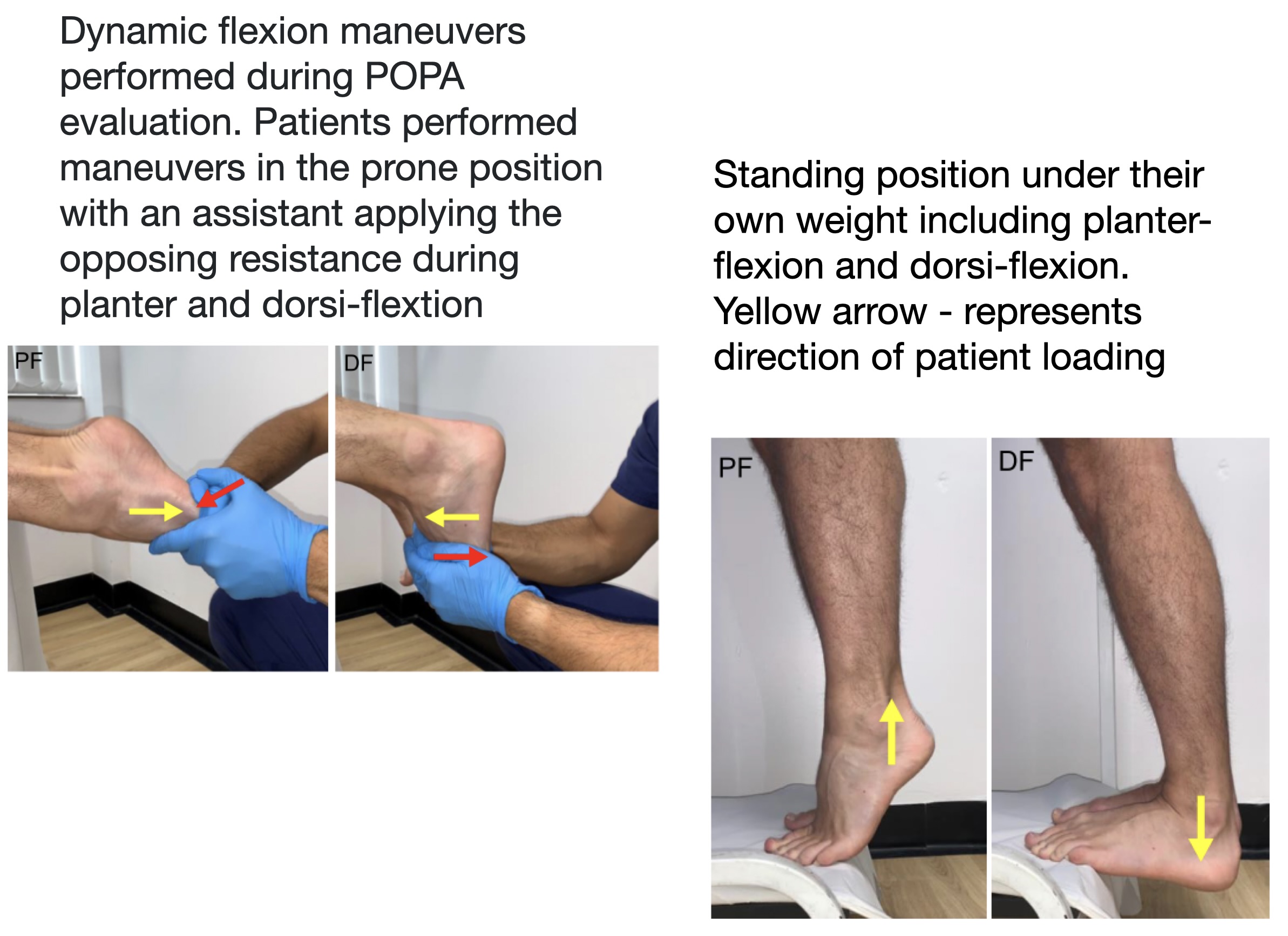
The problem: dynamic disease in a static imaging world
PAES is fundamentally a dynamic problem: the artery is fine at rest but compressed when the calf muscles contract. Traditional imaging - static CTA, MRA, or resting duplex - can easily miss purely functional entrapment, especially in early disease. That is exactly why dynamic duplex has become so important.
In one contemporary series, popliteal PSV nearly doubled - from 78 to 175 cm/s - during forced plantarflexion in affected limbs, with complete flow loss in many extremities. Other work in functional PAES shows that almost all surgically treated limbs have positive dynamic duplex when an optimized protocol is used, even if CTA or MRI are still read as “normal.”
How to scan these patients
For vascular sonographer and physicians, PAES requires a different mindset: scan like a stress test, not a static carotid.
• Start prone to map the vessel: define proximal and distal popliteal segments, measure baseline PSV, and look for fixed stenosis or aneurysm that hints at chronic entrapment.
• Then stand them up. The erect phase is where functional PAES declares itself. Image the distal popliteal artery in long axis and have the patient plantarflex and dorsiflex, ideally against resistance.
• Watch the color signal and waveform in real time: does PSV spike? Does the waveform collapse? Does flow disappear completely and then return as soon as the ankle relaxes?
A positive study is not just a pretty color image - it is a reproducible hemodynamic event: marked PSV rise or occlusion in the symptomatic limb, captured in erect maneuvers, with the patient saying, “That’s my pain.”
Avoiding the trap of overcalling
One of the most interesting recent findings: plenty of healthy people occlude their distal popliteal artery in the prone position during maximal plantarflexion. If we called PAES every time color dropped out prone, the incidence would explode overnight.
The key is context:
• Prone occlusion alone is common and nonspecific.
• Standing, symptom‑linked occlusion with abnormal waveforms and PSV changes is what matters.
This nuance is why PAES duplex needs a standardized protocol and consistent reporting language.
Where duplex fits among other imaging
Dynamic duplex is not meant to do everything - but it does a few things better than any other modality:
• It proves that the artery is functionally compromised in real time.
• It guides who should go on to dynamic CTA/MRA for anatomic mapping and, ultimately, dynamic angiography for definitive confirmation and treatment planning.
• It can even be used intraoperatively to confirm that decompression was complete.
CTA and MRA then define the relationship between artery and muscle, characterize stenosis or aneurysm, and help the surgeon plan the incision, muscle resection, and any necessary reconstruction. Angiography is reserved for when intervention is likely or the diagnosis remains uncertain.
Why this matters now
Functional PAES is being recognized more often, especially in competitive athletes and physically active young adults. Surgical decompression yields high rates of symptom improvement and durable patency when performed before major arterial damage, but redo operations are less successful. That makes the duplex lab the real front line: if the dynamic protocol is weak, these patients slip through; if it is strong, they get to the right surgeon at the right time.
For vascular practices, PAES is an opportunity to:
• Differentiate your lab by offering a formal functional PAES protocol.
• Educate referring sports medicine, orthopedics, and primary care colleagues about this under‑recognized cause of calf pain.
• Capture clinically meaningful pathology before it evolves into acute limb ischemia in a young, otherwise healthy patient.
Dynamic duplex is the bridge between a vague, frustrating symptom story and a precise, fixable diagnosis. In PAES, it doesn’t replace other imaging - it makes every CTA, MRA, and angiogram smarter. If your lab can reliably reproduce symptoms, document standing waveform changes, and use consistent, standardized reporting language, you stop calling it “mystery calf pain” and start calling it popliteal artery entrapment syndrome. The question isn’t whether PAES is out there; it’s whether your current duplex protocol is capable of consistently finding it!
